Padel is one of the fastest-growing sports in Southeast Asia — and for good reason. It is social, fast-paced, and easy to pick up. But as more players step onto the court, physiotherapists and orthopedic surgeons are beginning to see a rise in padel-related injuries.
In the latest episode of PhysioActive’s Singapore Surgeon Insight series, orthopedic surgeon Dr. Kevin Yik from Elite Orthopedics Singapore shares findings from his clinical practice and the key things every padel player should know to stay safe on the court.
Why Padel Is Harder on the Body Than It Looks
Padel is best described as a mix of tennis and squash, played inside a glass-walled court.

It is dynamic and involves rapid changes of direction, overhead swings, and reactive lateral movements. This combination places real stress on the shoulders, elbows, wrists, knees, and ankles — even during casual play.
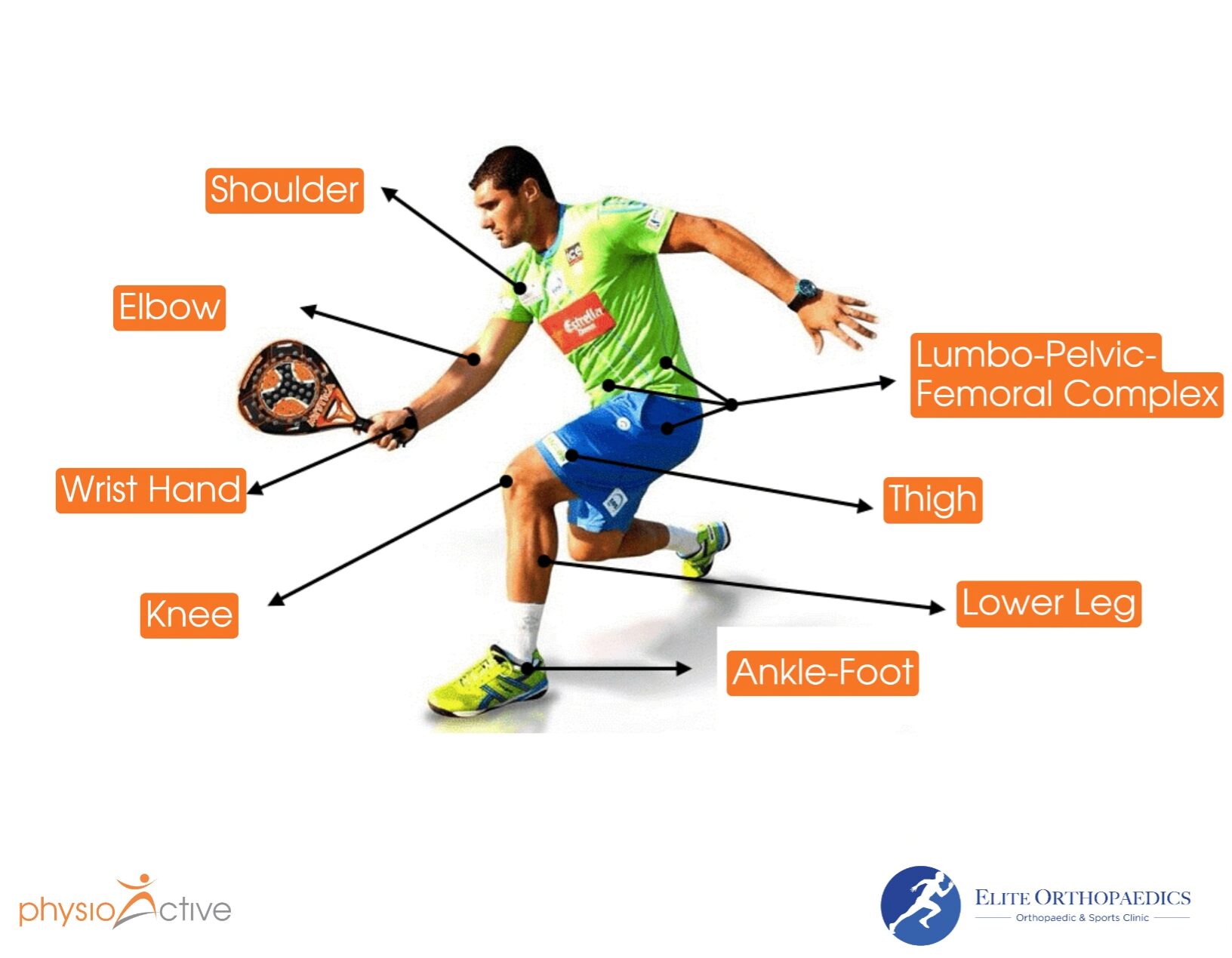
Unlike straight-line sports such as running, padel demands multi-directional agility. Your joints absorb forces from sudden stops, pivots, and lunges — often on hard court surfaces.
Common Padel Injuries: Beginners vs Experienced Players
Dr. Yik sees injuries across all skill levels, but the patterns differ.
Beginners
New players tend to compensate with poor technique — over-relying on the wrist or placing excessive strain on the elbow. Common issues include:
- Wrist ligament injuries and TFCC tears
- Tennis elbow or golfer’s elbow
Experienced Players
For more skilled players, technique is usually not the main issue. The more common problem is playing too frequently without adequate recovery. Overuse injuries are the primary concern:
- Rotator cuff tears in the shoulder
- Tennis elbow or golfer’s elbow
- Patellar tendonitis in the knee
- Plantar fasciitis in the heel
Acute injuries can happen to anyone. Falls, awkward twisting movements, and sudden changes of direction can cause ACL tears, meniscus tears, and Achilles tendon injuries.
When Should You Stop Playing and See a Doctor?
Most minor pain will improve with rest, ice, and elevation. However, Dr. Yik advises seeking a professional assessment if pain persists for more than one to two weeks despite rest.
Some symptoms require more urgent attention:
- Joint swelling
- Locking or jamming of the joint
- A feeling of instability — the joint feels loose or gives way
- Difficulty bearing weight, standing, or walking
If you experience any of the above, do not wait. Early assessment can prevent a small problem from developing into a serious injury.
Imaging, Injections, and Surgery: What You Need to Know
X-rays and MRI scans are standard tools for evaluating persistent or concerning symptoms. Beyond imaging, treatment options range from conservative to surgical.
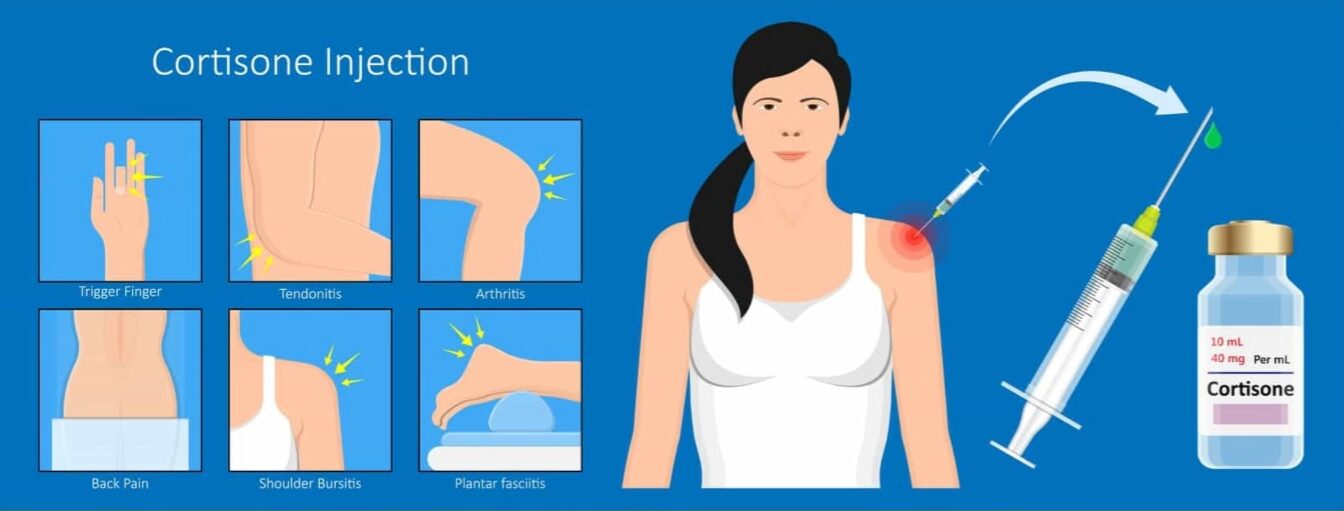
Steroid injections can help relieve pain and reduce inflammation in conditions such as frozen shoulder, though they are not always ideal when tissue healing is the primary goal.
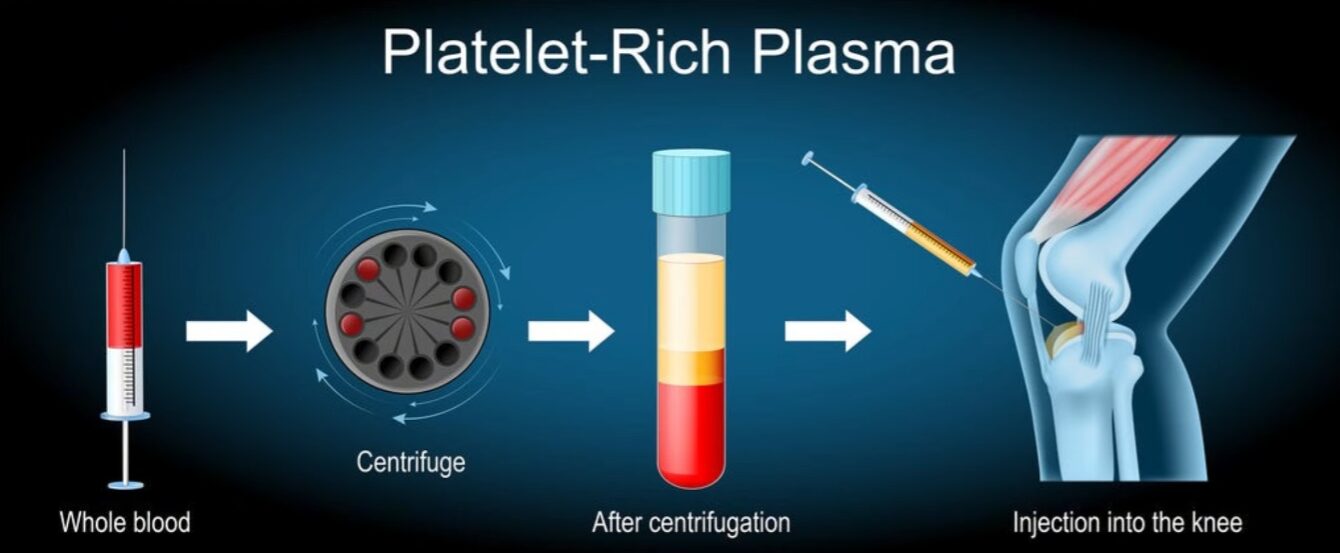
PRP (platelet-rich plasma) injections are increasingly popular. A small blood sample is taken from the patient, processed to concentrate the platelets, and injected into the injured area to stimulate the healing process. Many patients prefer PRP because it supports the body’s natural repair process rather than simply managing symptoms.
Dr. Yik emphasises that the majority of padel injuries respond well to non-operative treatment. Surgery is generally only considered after an adequate trial of conservative management — typically at least six to eight weeks of physiotherapy — has not produced the expected improvement.
The Role of Physiotherapy in Recovery and Prevention
Physiotherapy is the first-line treatment for most padel injuries. A structured rehabilitation programme focuses on two goals: relieving pain and rebuilding the endurance and tolerance needed to return to sport safely.
Beyond recovery, the exercises learned during physiotherapy sessions can be continued as a regular maintenance routine — keeping muscles conditioned and joints resilient so you can keep playing with a lower risk of re-injury.
Simple Prevention Tips for Every Padel Player
- Wear proper padel shoes. Padel shoes differ from tennis shoes — their sole pattern is designed for the multi-directional movements padel demands.
- Warm up before every session. Three to five minutes of light cardio such as jogging on the spot or jumping jacks is enough to raise your heart rate and prepare your muscles.
- Add dynamic stretches. Movements like arm circles, high kicks, and butt kicks mimic on-court actions and prepare your joints for play.
- Listen to your body. If symptoms persist for more than one to two weeks despite rest, get it checked. Early treatment is the best way to prevent a minor complaint from becoming a long-term problem.
Play Smart, Stay on the Court
Padel is a sport that rewards good technique, proper conditioning, and smart self-care. Whether you are new to the game or a regular on the court, the Physioactive team is here to help you recover from injuries and build the strength and resilience to keep playing at your best.
Contact Physioactive today to speak with our team about a padel injury rehabilitation or prevention programme tailored to your needs.